
Mental Health Parity Act Explained: Understanding Your Insurance Rights
When your insurance approves 20 physical therapy sessions without question but requires pre-authorization after just six therapy sessions for anxiety, it doesn’t just feel unfair it may actually be illegal. Understanding the mental health parity law is essential for anyone navigating insurance coverage for therapy, psychiatry, or substance use disorder treatment. When your copay for a primary care visit is $20 but $50 for a psychiatry appointment, you’re encountering exactly the kind of unequal treatment the Mental Health Parity and Addiction Equity Act was designed to prevent.
Navigating mental health insurance coverage can feel like facing an intentionally opaque system designed to deny care. Denials come without clear explanation. Appeals processes feel bureaucratic and intimidating. The mental health parity law exists specifically to protect you from these inequities. This guide explains what the law actually requires, which insurance plans must comply, how to recognize potential violations, and what steps you can take if you believe your rights are being violated.
What the Mental Health Parity Law Actually Requires
The Basic Principle: Equal Treatment, Not Unlimited Coverage
The Mental Health Parity and Addiction Equity Act of 2008 (MHPAEA), commonly called the mental health parity law, establishes one core requirement. If your health insurance plan offers both mental health/substance use disorder benefits and medical/surgical benefits, it must treat them equally when it comes to cost-sharing, treatment limitations, and access to care.

The mental health parity law doesn’t mean your insurance must cover all mental health treatment. It doesn’t eliminate copays, deductibles, or medical necessity requirements. What it does mean is that whatever rules, limits, and costs apply to your medical and surgical care must apply no more restrictively to your mental health and substance use disorder care.
If your plan covers outpatient medical care without requiring prior authorization, it generally can’t require prior authorization for outpatient mental health care. If your plan allows unlimited primary care visits, it can’t impose a session cap on therapy. According to guidance from the U.S. Department of Labor on mental health parity, the law requires comparability and fairness across benefit categories.
What “Parity” Means in Practice Under the Mental Health Parity Law
Parity operates across four key areas:
- Financial requirements: Deductibles, copayments, coinsurance, and out-of-pocket maximums for mental health care can be no more restrictive than those for medical/surgical care.
- Quantitative treatment limitations: Numerical limits like visit caps, day limits, or episode limits for mental health care must be no stricter than those for medical care.
- Non-quantitative treatment limitations: Policies and procedures like prior authorization, medical necessity criteria, formulary design, and network adequacy must apply comparably to mental health and medical/surgical benefits.
- Scope of benefits: If a plan covers mental health conditions in one classification of benefits (like outpatient care), the financial requirements and treatment limitations can’t be more restrictive than the predominant limits applied to medical/surgical benefits in that same classification.
A Brief History: Why the Mental Health Parity Law Was Needed
Before parity laws, it was common and legal for insurance plans to impose annual limits on mental health care (like a $10,000 cap per year) while offering unlimited coverage for medical care. Plans routinely capped therapy at 20 sessions per year while placing no limit on physical therapy or cardiology visits.
The original Mental Health Parity Act of 1996 prohibited annual and lifetime dollar limits on mental health benefits if a plan didn’t impose similar limits on medical benefits. But it was narrow, applying only to group plans with 50 or more employees.
The 2008 Mental Health Parity and Addiction Equity Act significantly expanded protections. It covered substance use disorder treatment and addressed not just dollar limits but also treatment limits, cost-sharing, and administrative practices. The Affordable Care Act (ACA) further strengthened the mental health parity law by requiring most individual and small group plans to cover mental health services as essential health benefits.
Federal Law vs. State Protections: How They Work Together
Federal mental health parity law sets a national floor. States can and many do enact stronger mental health parity protections. State laws may apply to plans exempt from federal requirements, mandate coverage of specific treatments, or provide more robust enforcement mechanisms.
When both federal and state laws apply, your plan must comply with whichever is more protective. If you believe your rights are being violated, checking your state’s specific parity protections can reveal additional rights beyond federal law. This connects to broader themes of understanding preventive checkups and insurance coverage.
Which Insurance Plans Must Comply with the Mental Health Parity Law
Employer-Sponsored Group Health Plans
Most employer-sponsored group health plans must comply with the mental health parity law. This includes plans offered by private employers, state and local government employers, and many non-federal governmental employers.
However, important exemptions exist:
- Small employer plans: Plans from employers with 50 or fewer employees are exempt from federal requirements (though state laws may still apply)
- Self-insured governmental plans: Some may be exempt
- Increased cost exemption: Plans can apply for exemption if compliance increases costs by 2% or more in the first year (rarely granted)
Marketplace Plans (ACA and the Mental Health Parity Law)
Health insurance plans sold through the Health Insurance Marketplace must comply with the mental health parity law. The ACA requires these plans to cover mental health and substance use disorder services as essential health benefits.
If you purchased your insurance through HealthCare.gov or a state marketplace, parity protections apply.
Medicaid Managed Care Plans
Medicaid managed care plans where states contract with private insurers to provide Medicaid benefits are subject to the mental health parity law. Traditional fee-for-service Medicaid is not, though states may have their own parity policies.
Plans Exempt from the Mental Health Parity Law
Several types of coverage are not subject to federal parity requirements:
- Plans from employers with 50 or fewer employees (unless state law requires parity)
- Grandfathered health plans
- Retiree-only plans
- Plans that don’t offer mental health benefits at all
- Medicare (though Medicare has its own mental health coverage rules)
- TRICARE (military health coverage has separate policies)
How to Find Out if Your Plan Must Comply
Check your plan’s Summary of Benefits and Coverage (SBC) or contact your insurance company directly. Ask:
- “Is this plan subject to the Mental Health Parity and Addiction Equity Act?”
- “Does this plan comply with federal and state mental health parity requirements?”
Your plan administrator or HR benefits office can also confirm coverage. For those exploring therapy options, our therapy cost comparison provides additional context on mental health coverage considerations.
Common Violations of the Mental Health Parity Law
More Restrictive Session Limits for Therapy Than Physical Therapy
If your plan covers unlimited physical therapy visits but caps mental health therapy at a specific number of sessions per year, that’s likely a violation of the mental health parity law.
Red flag: Your plan says “20 outpatient mental health visits per year” but doesn’t impose similar limits on other outpatient specialty care.
Higher Copays for Mental Health Visits Than Primary Care
If you pay a $20 copay for a primary care visit but a $50 copay for a therapy or psychiatry visit, and this discrepancy isn’t based on a consistent specialist vs. generalist distinction applied equally across all care, it may violate the mental health parity law.
Red flag: Mental health copays are categorically higher than comparable medical visit copays.
Stricter Prior Authorization for Mental Health Than Medical Care
If your plan requires prior authorization for outpatient mental health treatment after a small number of sessions but doesn’t require comparable authorization for ongoing outpatient medical treatment, that’s a potential violation.
Red flag: You need insurer approval to continue therapy after six sessions, but you can see a cardiologist or physical therapist repeatedly without pre-authorization.
Narrower Provider Networks for Mental Health
If your plan has hundreds of in-network primary care doctors but very few in-network therapists or psychiatrists forcing you to travel long distances or wait months for appointments this may violate the mental health parity law’s network adequacy requirements.

Red flag: You have dozens of in-network orthopedic surgeons within 10 miles but only two in-network psychiatrists within 50 miles.
More Stringent Medical Necessity Criteria
If your plan applies stricter standards for determining whether mental health treatment is “medically necessary” than it does for medical treatment, that’s a potential violation.
Red flag: Your therapist’s treatment plan is repeatedly questioned or denied while comparable ongoing medical treatment is routinely approved.
What the Mental Health Parity Law Does NOT Guarantee
Parity Doesn’t Mean All Mental Health Treatment Must Be Covered
The mental health parity law requires equal treatment, not unlimited coverage. Your plan can still:
- Define which mental health conditions and treatments are covered
- Establish medical necessity criteria (as long as they’re comparable to medical care)
- Exclude certain treatments deemed experimental
- Require care from licensed, qualified providers
Your Plan Can Still Deny Coverage for Medical Necessity Reasons
Your insurance company can still determine that requested mental health treatment isn’t medically necessary. But it must apply the same rigor and standards to mental health as it does for medical/surgical care.
A denial based on medical necessity isn’t automatically a violation of the mental health parity law. However, if mental health claims are denied at much higher rates, that may indicate a parity violation.
You May Still Have Out-of-Pocket Costs
The mental health parity law doesn’t eliminate deductibles, copays, or coinsurance. It just requires that those costs be no higher for mental health care than for comparable medical care.
How to Check If Your Insurance Complies with the Mental Health Parity Law
Comparing Mental Health and Medical/Surgical Benefits Side-by-Side
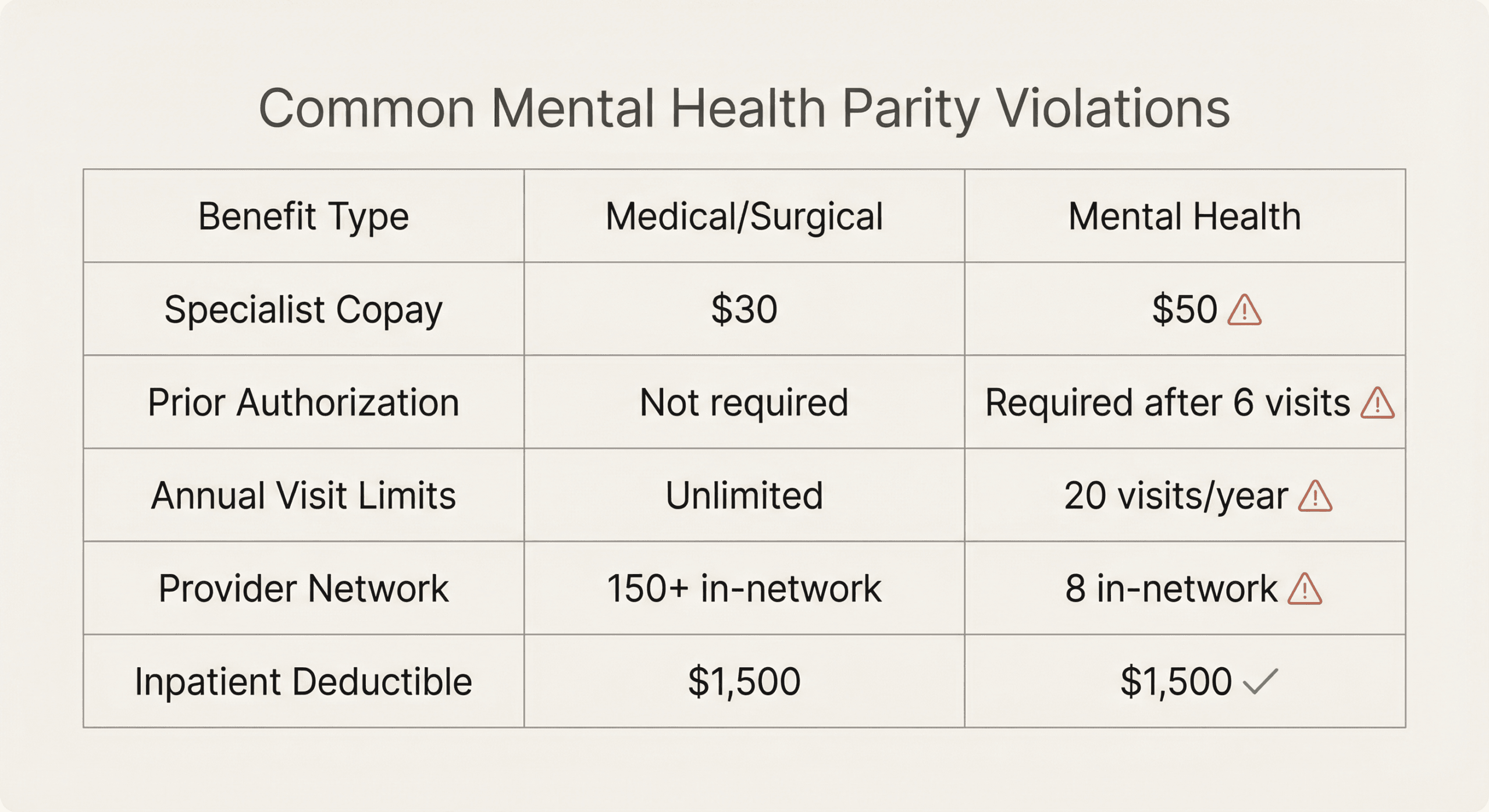
This side-by-side view makes disparities easier to identify.
Questions to Ask Your Insurance Company
Call your insurer’s customer service line and ask:
- “Does this plan comply with the Mental Health Parity and Addiction Equity Act?”
- “Why is my copay for therapy higher than my copay for other specialist visits?”
- “Why does mental health care require prior authorization when similar outpatient medical care doesn’t?”
- “How many in-network mental health providers are there in my area compared to medical specialists?”
Take notes on who you spoke with, the date and time, and what they said.
Documenting Potential Violations
Keep records of:
- Explanation of Benefits (EOB) statements showing denied or limited mental health claims
- Denial letters with stated reasons
- Prior authorization requests and responses
- Notes from calls with your insurance company
- Your plan documents
- Comparisons between mental health vs. medical care treatment
This documentation will be essential if you file an appeal or complaint. Understanding when to seek professional support for anxiety becomes easier when you understand your insurance rights.
What to Do If You Think the Mental Health Parity Law Is Being Violated
Step 1: Contact Your Insurance Company
Start by calling your insurer and asking for a clear explanation of the discrepancy. Request explanations in writing.
Step 2: File an Internal Appeal
If you’ve been denied mental health coverage or believe your plan violates the mental health parity law, file an internal appeal. In your appeal:

- Explain why you believe the denial violates parity
- Provide side-by-side comparisons showing disparate treatment
- Cite the Mental Health Parity and Addiction Equity Act
- Include supporting documentation
Insurance companies must respond within specific timeframes (typically 30 days for standard appeals, 72 hours for urgent appeals).
Step 3: Request an External Review
If your internal appeal is denied, you have the right to an external review by an independent third party at no cost to you.
Step 4: File a Complaint with Your State Insurance Department
Every state has an insurance department that handles consumer complaints. State insurance departments can investigate, require corrective action, and impose penalties.
Step 5: File a Complaint with Federal Agencies
You can also file complaints with:
- U.S. Department of Labor (DOL): For employer-sponsored ERISA plans
- Centers for Medicare & Medicaid Services (CMS): For Marketplace plans
Step 6: When to Consider Legal Assistance
Consider consulting a patient advocate or healthcare attorney when:
- Your claim involves significant financial stakes
- You’ve exhausted internal appeals without resolution
- You believe your plan systematically violates parity
- You’re facing complex legal questions about your rights
Resources for Help with Mental Health Parity Law Issues
Federal Resources
U.S. Department of Labor – Employee Benefits Security Administration:
- Oversees parity compliance for ERISA employer-sponsored plans
- Online complaint filing: dol.gov/agencies/ebsa
Centers for Medicare & Medicaid Services (CMS):
- Oversees parity for Marketplace plans and Medicaid managed care
Nonprofit Advocacy Organizations
National Alliance on Mental Illness (NAMI):
- Mental health parity resources, advocacy, and support
- HelpLine: 1-800-950-NAMI (6264)
Mental Health America (MHA):
- Parity information, advocacy toolkit, and policy updates
The Kennedy Forum:
- Leading parity advocacy organization
- Tracks enforcement and publishes compliance reports
State Insurance Departments
Every state has an insurance department that handles consumer complaints, including parity violations. Find yours through the National Association of Insurance Commissioners (NAIC) website or by searching “[Your State] insurance department.”
Frequently Asked Questions About the Mental Health Parity Law
Does the mental health parity law mean my insurance has to cover therapy?
Not exactly. The mental health parity law requires that if your plan covers mental health benefits, it must treat them equally to medical benefits. ACA-compliant plans must include mental health as an essential health benefit.
Can my insurance still limit the number of therapy sessions?
Yes, but only if it applies similar limits to medical care. If your plan caps therapy at 20 sessions per year, it must apply comparable limits to similar medical treatments. If it doesn’t, that’s likely a violation of the mental health parity law.
What if my therapist isn’t in-network?
The mental health parity law doesn’t require your plan to contract with any specific provider. But it does require that your access to in-network mental health providers be comparable to your access to in-network medical providers.
Does the mental health parity law apply to substance use disorder treatment?
Yes. The Mental Health Parity and Addiction Equity Act applies equally to substance use disorder benefits. All the same protections equal cost-sharing, comparable treatment limits, and equivalent access apply to addiction treatment.

Can I be penalized for challenging my insurance company?
No. You have legal rights to appeal denials, file complaints, and advocate for parity compliance. Insurance companies cannot retaliate against you for asserting your rights.
Important Information and Disclaimers
Understanding the Scope and Limits of This Guide
This article provides educational information about the mental health parity law and related protections. It is not legal advice. Insurance coverage situations vary based on plan type, state law, specific circumstances, and evolving regulations.
The mental health parity law requires equal treatment of mental health and medical/surgical benefits, but it doesn’t mandate that specific treatments be covered. Coverage decisions depend on your specific plan, medical necessity determinations, and individual circumstances.
When to Seek Professional Support
For guidance on your specific situation, consult your insurance company, state insurance department, a patient advocate, or an attorney specializing in healthcare law. Many resources mentioned in this guide offer free or low-cost support.
Staying Informed About Policy Changes
Mental health parity enforcement continues to evolve. Stay informed by:
- Monitoring updates from the DOL, CMS, and HHS
- Following NAMI, Mental Health America, and The Kennedy Forum
- Checking your state insurance department’s website
- Reviewing your plan documents annually during open enrollment
Takeaway
The mental health parity law exists to protect you from unequal treatment of mental health and medical coverage. Understanding the mental health parity law empowers you to recognize when your insurance isn’t treating your mental health benefits fairly. If your plan imposes higher copays, stricter session limits, or more burdensome authorization requirements for mental health than for medical care, you have the right to challenge those practices. Document disparities, file appeals, and contact your state insurance department or federal agencies when needed. The mental health parity law doesn’t guarantee unlimited coverage, but it does guarantee fairness and knowing your rights is the first step toward asserting them.
This content does not substitute for legal advice. For guidance on your specific situation, consult a qualified professional.
